
Edward J. Safra Family Lodge, on the grounds of the National Institutes of Health, Bethesda, MD
My diagnosis of prostate cancer came as a rude jolt in the winter of 2007. Yet when I look back on the sequence of events that began the moment my urologist delivered the terrible news, I do not find myself filled with recollections of vulnerability, fear, and pain. Instead, I remember a special time in which I received top-notch medical care, combined with the warmth and love of family. I remember with unusual vividness and fondness the books I read while in the hospital and during the days and early weeks of recovery. I recall the routes of some of the walks I took, and the way the spring flowers and vegetation looked. How would I sum up my feelings when I look back on my encounter with prostate cancer? I would say it brings back a warm glow.
Jacob and I had our baseball mitts with us. During my recovery, after I moved into the Family Lodge with them, we played catch on the lawn, trying not to let the ball go into the flower beds.
To be sure, fear and pain and vulnerability were all part of the experience. How could you not experience fear when you’ve been handed at best a major disruption of your life, and at worst, a possible death sentence? In between the best and the worst are a continuum of possibilities such as full longevity but with compromised command of bladder, bowels, and/or sexual functioning.
There was pain embedded within each part of the experience. The urologist compared the biopsy to firing a pop gun at your testicles—and that was accurate. Before my surgery, there was an MRI, in which a balloon containing a camera was placed deep inside the only bodily cavity that is located adjacent to the prostate. That lasted about 40 minutes and not one second of that was comfortable. Then there was the pain after the surgery. The anesthesiologist had forewarned me that nothing would happen during surgery to my upper body, and yet, a certain proportion of men would feel intense shoulder pain. It turned out I was one of them. From her explanation, I understood that it was “referred pain.” But it still hurt! So much that it took about 10 days before I could roll over on that side of my body. For the first few days, I needed opiates to avoid calling out in pain.
Was there vulnerability as well as fear and pain? Yes, that too. A nurse drawing blood. A nurse hooking me up on IV fluids. A nurse giving me my opiates. A nurse standing next to me while I tried to pee.
So, what about that warm glow?
It started with my arrival at the Mark O. Hatfield Clinical Center of the National Institutes of Health (NIH), in Bethesda, Maryland. Betty and I immediately sensed we were entering an environment that was extraordinary in its medical resources but also in other ways. I took as a good omen that the building bore the name of an antiwar Senator from Oregon whom I remembered from the Viet Nam era. The entryway with its distinctive glass and steel overhang presented a pristine, contemporary look that seemed at once both audacious and welcoming. There were friendly people, greeting us at information desks and right beyond them was the Au Bon Pain, holding a strategic spot in the downstairs foyer,
The real sense of joy came upon heading up the elevator to meet Dr. Pinto and his associates. I didn’t go there as a prospective patient; through a family connection, I was fortunate to have secured a consultation. That’s all we were expecting, and I was hoping these experts standing at the pinnacle of cancer research would steer me toward the right procedure, and the best hospital in which to do it—most probably, we thought, in New York or Boston.
It turned out they could do better than that: I could have the surgery right there, so long as I consented to return (at their expense) for the next five years and be examined and answer questions about my bladder, my bowels, and my sexual functioning. You don’t get to be a patient at the NIH Clinical Center unless you are recruited as a participant in a study, and I was being recruited for a “quality of life” study. This would be my ticket to enter the gates of this magical campus.
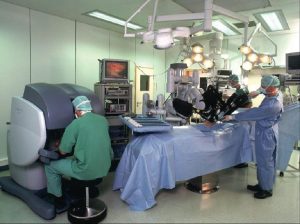
Dr. Pinto would be at the controls of the DaVinci robot, while another doctor, a surgical fellow, would be at my side giving him the play-by-play.
The surgical procedure would be a laparoscopic-robotic prostatectomy. If the margins were clear (no cancerous cells found on the outside of the organ upon its removal) there would be no chemo or radiation or any other medical procedures. We scheduled my surgery for the first week of May (about 7 weeks down the road). That would enable my prostate to heal from the biopsy and me to finish my first spring semester of full-time college teaching.
If the warm glow got its start in encountering competence, experience, and professionalism in every interaction with the staff of the NIH, it really began to kick in more strongly when we learned about the Edward J. Safra Family Lodge and found out that Dr. Pinto could secure us a reservation for a room there. Right on the NIH campus, and opened just two years earlier (2005), it was an attractive building of wood and stone, designed in the style of a 1900 English Arts and Crafts Manor, a 10-minute walk (or a short shuttle ride for those who could not walk) from the Clinical Center. It would mean Betty and Jacob (or anyone else who came to attend to me during my recovery) would have a comfortable place to stay, with no charge for lodging or even for parking, no commute from a hotel to the NIH in the morning, no driving back, drained and concerned, in Washington, DC, traffic in the evening. Once I was discharged, t

Not our room, but this is what our room looked like. I shared it first with Betty and Jacob, then with my sister, then my brother.
he Family Lodge is also where I would stay. (I could not fly home until I had my catheter removed, anticipated to be seven days after surgery if all went smoothly.)
The Lodge provided breakfast cereals, pastries, milk, tea, and coffee for free to all residing there. In addition, there were multiple stoves and microwave ovens available for cooking, and each of us would be assigned a shelf within a refrigeration unit that took up an entire wall of the common kitchen. This is where Betty would keep the fresh strawberries and other treats I so fondly recall.
The formidable medical staff and facilities were the first necessity for a successful surgery. Finding such a wonderful lodging situation eased many of our worries about the circumstances we were facing. But most central to the recollection of the warm glow was the love and support of my family during that time.
Jacob, at age six, did not understand, as he told me many years later, “what cancer was.” He was just excited to be in a city where he could spend time with his cousins! And that’s just the way we wanted it. Betty’s brother Josh and his wife Teresa had three boys just a little older than Jacob. Both parents worked at the NIH; they were the “family connection” that secured us the initial consult.
Betty was my knowledgeable and gracious partner at every step and at each decision point from the time I got the diagnosis. She must have buried her own anxieties very well, because I only remember her as a font of warm support and sound advice. She even advised me whom to speak with among my colleagues and how to talk to my department chair. (She had been in an academic setting for over 15 years, while I was just starting.)
During the surgery, she had to sit in the waiting room for over four hours, wondering how I was doing—and meanwhile, keeping a very active, talkative and endlessly inquisitive son amused. The games and puzzles available to families in the waiting area only engaged Jacob for so long. The rest of the time, s
he had to make up on her own ways to keep him from bouncing off the walls. After the surgery, Betty was juggling care for me with care for our son, back and forth between her brother’s home in Bethesda, where Jacob spent some of his time, and the Clinical Center.
Jacob and I had our baseball mitts with us. During my recovery, after I moved into the Family Lodge with them, we played catch on the lawn, trying not to let the ball go into the flower beds. It was May, so the weather was warm in Maryland, and we were dressed in shorts. The tube running from my catheter protruded below the end of my shorts on my left leg. But he didn’t care and neither did I. We watched baseball games on TV in the Lodge with other families. By luck, the local team, the Baltimore Orioles, were hosting the Boston Red Sox for a three-game series, so we could, along with other families staying in the Lodge, watch the games on TV. Jacob already knew the names of Dustin Pedroia, Jacoby Ellsbury, Coco Crisp, and many others.
He and I also sneaked over one afternoon into the “Children’s Inn.” This was another lodge, not far away on the campus, but specifically for the families of children being treated at the Clinical Center–while the Family Lodge was for families of adults. The Children’s Village had one asset that we lacked–video games! So Jacob and I went over there the one time and played NBA 2K and a couple other games ( no tokens or coins required; everything was free). He crushed me.
We didn’t want Jacob to miss a whole week of Kindergarten, and Betty needed to return, once I was in recovery, to resume her teaching and the supervision of students in her lab. My sister Elaine flew in from Ohio, interrupting her law practice to spend some days with me, allowing Betty and Jacob to head home. When Elaine had to go back, my brother Leon flew in from Chicago, taking time from his university teaching, staying until the day I got my catheter removed and I could head to the airport and return home. Betty had handled the communication to work out this whole complicated schedule well in advance of the surgery.
My days with Elaine and then Leon were filled with reading, taking walks, talking, and doing a fair amount of sleeping. Our days moved slowly. I hope they each got some reading or other work done on their laptops. It was the most one-on-one time I had with either of them in many years. I felt cherished and was beyond grateful.
In the days right before and after the surgery, while staying in the Clinical Center, I was reading a novel Betty gave me by Dai Sieje titled, Balzac and the Little Chinese Seamstress. It concerned two high school-aged boys from well-to-do city families who are sent out to the countryside to do agricultural work during the Cultural Revolution in China.
At some point during the evening, rather late, the second day after the surgery, I took a break from reading, and went for a walk around my floor, pushing the cart with my IV tubes in front of me. I was aware as I passed other rooms that most patients were sleeping. I sensed that the staff who were around were in a relaxed state of mind, and this insight was confirmed when a friendly woman wearing the usual hospital whites and a name tag, perhaps in her mid-30s, came from behind one of the stations to ask how I was doing and initiate a bit of a chat. I learned from our conversation that she was a phlebotomist (one who specializes in drawing blood), and that she had immigrated from China. I told her I was reading a novel that was set during the Cultural Revolution, and she told me some details I no longer recall about her own extended family’s experience of the Cultural Revolution.
When she learned I was a professor of special education, she told me about her daughter, who was diagnosed as an “elective mute” (i.e., someone who has displayed the capacity to speak but who has ceased to speak). She asked me if I knew anything about that condition, and I told her of a very rewarding experience I had earlier in my career when I was a teacher in a child care center, and I worked with a four-year-old named Charlie who presented that same condition. She asked if I had any strategies to suggest, and I did suggest a few. How amazing it was in that moment to be treated as a professional with some guidance to offer, instead of just a man who was pushing around an IV cart and needed help to carry out his most basic functions! It felt surreal, but wonderful.
While making my circuit of the floor, I was wearing a red silk gown that my mother had given me from a trip she took in the 1980s, one I had only rarely worn, so that it still looked quite new. It had a large Chinese symbol in gold on the back, the meaning of which I had never known. The phlebotomist asked if I knew what it meant. I said I had no idea. She told me that it was the symbol for “long life.”
Now do you see why I feel such a warm glow when I look back on my encounter with prostate cancer?
Dale Borman Fink retired in 2020 from Massachusetts College of Liberal Arts in North Adams, MA, where he taught courses related to research methods, early childhood education, special education, and children’s literature. Prior to that he was involved in childcare, after-school care, and support for the families of children with disabilities. Among his books are Making a Place for Kids with Disabilities (2000) Control the Climate, Not the Children: Discipline in School Age Care (1995), and a children’s book, Mr. Silver and Mrs. Gold (1980). In 2018, he edited a volume of his father's recollections, called SHOPKEEPER'S SON.






Dale, your story really resonated with me. Four years ago, my husband had prostate cancer surgery. Most of it was totally lemons, including the frightful moment my daughter and I were brought into a small room to talk to the doctor post-surgery. There had been a complication, but he was fine. Of course, we both thought he had died because the nurse just told us to wait there. I could relate to the closeness we felt during his recovery period. It was hard for him, but we made it through with lots of love and support from our daughter who lives near us and our friends.
Thanks for sharing this. OMG I can imagine those moments of tense waiting after the nurse didn’t tell you anything.
Dale, this is a great story of how the most intensely negative and positive circumstances can coexist. I am glad that you recovered. It’s amazing the details one remembers during such a time. I have many memories of the two weeks when Dick became ill on a cruise, our evacuation from the ship through Mexico, and his and my time in San Diego first at the hospital and then at a hotel before we could fly home. What do I remember most? The best pork tacos I ever ate. Life is funny that way.
I love that you are not afraid of remembering those delicious tacos! It is important to be able to validate the positive even in the most catastrophic situations. In my case, I am fortunate that in the end, there was no catastrophe but a lot of warm memories.
Thank goodness you’re well now Dale, and thank you for sharing your story of the competent medical team and the loving family that helped turn your bitter diagnosis and your bout with cancer into a sweeter memory.
Such a beautifully written story, Dale, starting with your title reminiscent of Love in the Time of Cholera. Your story is much more upbeat than that one, where it takes 50 years for the protagonists to find happiness. The NIH Clinical Center and its Family Lodge sound like a dream come true – you were so fortunate to get your care there. That, and the care from your devoted family, was certainly some sweet lemonade.
I was hoping someone would notice and comment on the Garcia Marquez reference. Thanks for that and all your comments.
Ah, Love in the Time of Cholera,
and you didn’t have to wait all those years for the love!
Such a detailed and intimate story, Dale. How wonderful that you were able to be treated at NIH, get such great care, then spend precious time with your siblings as well as your wife and Jacob (I love how you mention the Red Sox players – those names brought back specific memories for me too). You do not shy away from sharing your difficult, painful moments, but have transformed them into glowing, positive memories; truly lemonade moments.
35 years ago, my brother-in-law was diagnosed with aplastic anemia. None of his immediate relatives were bone marrow matches but he lived in Washington, DC at the time and got into an experimental treatment program at NIH. It saved his life and, just as you described, he had to go back for at least 5 years for check-ups (I believe in his case it was even longer). 35 years later, he is still doing well. I hope you continue to thrive as well.
You describe both lemons and lemonade so well, and how the two can co-exist. It sometimes takes a dramatic event to bring out the love that is in our lives, and what a wonderful experience that can be. So easy to get caught up in the day-to-day. What a gift to live more fully, despite (or because of) the circumstances.